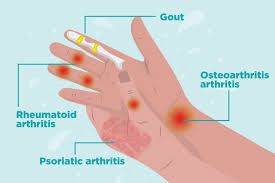
Rheumatoid Arthritis
The presence of inflammation and redness along with pain and swelling in several joints is a hallmark of arthritis. Commonly affected are the hands, knees, elbows, fingers, and wrists. Other joints can also be affected and this disease also has an autoimmune aspect. While there are several types of arthritis, Rheumatoid and Osteoarthritis are the most common. Patients suffering from this disease should be encouraged to seek regular medical care and have a complete metabolic and blood workup, as well as a specific test for antibodies commonly found in patients who have arthritis. While it is relatively simple to see that your joints are painful, the exact cause could be related to age, stress, diet, infection, overuse, autoimmune disease, or causes that are unknown and undiagnosed.
Osteoarthritis is the most common form of the disease and predominantly affects the synovial joints, particularly the knees and hips. This allows for the degeneration of the cartilage and the underlying subchondral bone to which the cartilage is attached. While it is a degenerative, progressive disease that can occur with age or overuse of the joints, there is also a hereditary component. Arthritis is the leading cause of chronic disability in the US, and many patients suffer from pain and limited function due to this disease.
Rheumatoid arthritis is a chronic and systemic disease, and can usually be determined by testing for the presence of the RA factor in one’s blood. Sometimes this diagnosis may require several visits to the doctor or tests over time to accurately determine the diagnosis of RA. The inflammation and pain in RA usually can affect the hands, feet, and spine as well as the shoulders and knees. Redness, stiffness, swelling, excess synovial fluid, and pain are characteristic of the disease, as well as other systemic conditions such as dry eyes, mouth, and limited saliva. In this disease, inflammation can also affect the lining of your heart (pericardium) and lungs (pleura). Joints can become swollen, painful, and limited motion is possible.
The inflammatory response, as well as the autoimmune response, are areas in which excess chemicals are produced that cause further joint damage and destruction. These chemicals usually involve cytokines, proteases, and chemokines which lead to cartilage degradation. Cannabinoids have been shown to be effective is limiting some of these harmful compounds, reducing inflammation thereby limiting the destruction of cartilage and progression of the disease. Also, the ability of cannabis to reduce pain and the perception of pain is also a beneficial effect of cannabinoids in helping patients cope with this disease.
While more research needs to be conducted in determining the most beneficial cannabinoids useful in treating this disease, it has become apparent that CBD is an important cannabinoid in blocking the progression of the disease in laboratory animals. Some studies report a 70% decrease in pain and joint damage. However, the exact dose of CBD to treat arthritis can vary and requires further study as CBD is biphasic and the effects of CBD are dose-dependent. Raising the dose level of CBD often can produce opposite effects, and become counter-productive, therefore more CBD is not always better!! CBD works to reduce arthritic inflammation through several chemo metabolic pathways involving the following:
*Reduction of collagen specific antibodies
*Suppression of lymphocytic proliferation in the disease
*Immunosuppression and immune modulation
*Reduction of Tissue Necrosing Factor (TNF-alpha)
*Blockage of nitric oxide production by macrophages
*Reduction of free radicals (anti-oxidants)
*Stimulation of chondrocyte precursor cells to aid in the production of new cartilage
Cannabinoids and the endocannabinoid system have shown to be important modulators of bone density, growth, and repair.
Osteoclastic activity that causes bone and cartilage destruction is regulated through the endocannabinoid system, and reducing the activity of osteoclasts allows for joint and cartilage recovery and repair. This effect is modulated through the CB1 and CB2 receptors as well as the TRPV1, and PPAR receptors. CBG, or cannabigerol, may also play an important role in bone and joint metabolism and help stimulate new cartilage and bone formation but studies are scarce at this point in time on the other cannabinoids that play a role in helping to treat this disease. The role of THC in RA can be beneficial to be combined with CBD to achieve the well- known entourage effect – where the cannabinoids synergize and potentiate each other to provide maximum medicinal effect. It should be noted that the THC comes with ample psycho-activity not desired by some RA patients, and also can exacerbate dry mouth and dry eyes common in the disease. Ingestion techniques for cannabis use in arthritis can be smoking, vaping, edibles, tinctures, or topical applications applied for joint pain and swelling. Each patient may find a different technique or dosage that works best in their unique situation.
As cannabis is a very complex plant with over 600 known compounds, patients must experiment with different methods of use to find one that allows them to reduce pain and disability from the disease. Cannabis can be used after the traditional medication is employed, and is compatible with other holistic therapies for arthritis. These may involve yoga, acupuncture, physical therapy, water exercise, chiropractic care, laser therapy with low-level laser, and possibly diet and lifestyle changes. Any negative or detrimental effects of using cannabinoids to help treat this disease are related to excess psycho-activity of THC, the exacerbation of dry mouth and eyes, and some low-grade sedation caused by CBD. Otherwise, patients with arthritis should feel comfortable in using cannabinoids as part of their therapy in treating both Rheumatoid and Osteoarthritis.